Medical malpractice occurs when healthcare providers fail to meet the standard of care—the level of skill and diligence that a reasonably competent provider in the same specialty would exercise under similar circumstances—resulting in preventable harm to patients.
At Williams Elleby Howard & Easter, we investigate misdiagnosis, surgical errors, medication mistakes, birth injuries, anesthesia complications, and informed-consent failures to determine whether negligence caused your injury. If mistakes were made, we build cases backed by expert testimony that hold the negligent healthcare providers accountable.
Key Takeaways for Georgia Medical Malpractice Cases
- Diagnostic errors represent the leading cause of medical malpractice claims, with cancer, heart attacks, and infections most frequently missed or delayed.
- Georgia requires expert affidavits at the time you file suit, meaning you need a qualified medical expert willing to testify that the defendant breached the standard of care before your case even starts.
- Emergency-room malpractice claims face a higher “gross negligence” standard, requiring proof of willful or wanton misconduct rather than simple negligence.
- In most cases, you have two years from the date of injury (or when you discovered or should have discovered it) to file suit, with a five-year statute of repose barring claims filed more than five years after the negligent act.
- Georgia’s medical malpractice non-economic damages cap was struck down in 2010, so current Georgia law allows for full and fair pain and suffering awards.
Misdiagnosis and Delayed Diagnosis
Diagnostic errors, like misdiagnosis, delayed diagnosis, or failure to diagnose, consistently rank as the most common medical malpractice allegations nationwide. Cancer, cardiovascular events, and infections are the conditions most frequently missed or diagnosed too late to prevent serious harm.
Cancer Misdiagnosis
Breast cancer, lung cancer, colon cancer, and melanoma all present symptoms that primary care physicians and specialists sometimes attribute to less serious conditions.
Early-stage cancers respond to treatment with high survival rates. Late-stage cancers metastasize, require aggressive chemotherapy and radiation, and carry significantly lower five-year survival rates.
The difference between a stage-one diagnosis and a stage-four diagnosis could stem back to a provider who failed to order appropriate imaging, didn’t follow up on abnormal test results, or misread pathology reports.
Heart Attack and Stroke Misdiagnosis

Diagnostic protocols exist for chest pain and neurological symptoms. EKGs, troponin blood tests, CT scans, and stroke-assessment scales catch most life-threatening events when providers follow standard procedures.
Malpractice can occur when physicians skip these steps, misinterpret results, or discharge patients without appropriate monitoring.
Infection Misdiagnosis
Sepsis, meningitis, and post-surgical infections progress rapidly when undiagnosed. This could manifest as a fever and confusion dismissed as the flu, or post-operative abdominal pain attributed to routine healing, when in fact imaging would reveal an abscess.
Blood cultures, imaging, and laboratory tests help identify infections and guide the selection of antibiotic or antifungal medication.. Delays in ordering tests, failures to recognize early warning signs, or misreading lab results all may constitute diagnostic negligence when the standard of care required earlier intervention.
Surgical Errors and Wrong-Site Surgery
Surgical malpractice encompasses a range of preventable errors during operations, including operating on the wrong body part, leaving surgical instruments or sponges inside patients, damaging nerves or organs adjacent to the surgical site, or performing unnecessary procedures based on misdiagnosis.
Wrong Site, Wrong Patient, Wrong Procedure Events
Wrong-site surgery violates multiple safety protocols designed to prevent exactly these errors. The Joint Commission’s Universal Protocol requires surgical-site marking, pre-procedure verification, and team time-outs to be performed before incision. Yet, these “never events” still occur when providers skip steps or fail to speak up when something appears to be wrong.
Retained Surgical Objects
Sponges, clamps, retractors, and needles left inside body cavities after surgery cause infections, obstructions, and perforations. Surgical counts (tallying instruments and materials before closure) catch most retained objects. However, count errors, miscommunication between surgical nurses, or surgeons closing without proper verification can create malpractice liability.
Nerve and Organ Damage
Surgeons operating near critical structures sometimes cause permanent damage through poor technique, inadequate visualization, or failure to identify anatomy correctly. Not every complication constitutes negligence. However, damage that occurs because a surgeon deviates from accepted technique or fails to recognize and correct an error during the procedure may support malpractice claims.
Anesthesia Errors and Failure to Monitor
Anesthesiologists and certified registered nurse anesthetists (CRNAs) control patients’ airways, breathing, and vital signs during surgery. Errors in anesthesia administration, inadequate pre-operative evaluation, or failure to monitor patients properly cause brain damage, cardiac arrest, and death.
Dosing Errors and Drug Interactions
Administering too much anesthesia depresses respiration and cardiac function; too little allows patients to wake during surgery. Failing to account for patient weight, age, comorbidities, or drug interactions creates a risk of overdose or adverse reaction.
Intubation Complications
Difficult intubations delay oxygen delivery and cause hypoxic brain injuries when providers don’t recognize the problem quickly and switch to alternative airway management techniques. Esophageal intubations are fatal unless detected and corrected immediately.
Inadequate Monitoring
Anesthesia providers must continuously monitor oxygen saturation, heart rate, blood pressure, and end-tidal CO₂. Equipment failures, alarm fatigue, or providers leaving the operating room for non-emergent reasons all compromise patient safety. When monitoring lapses allow unrecognized hypoxia, patients suffer permanent brain damage or death.
Medication Errors
Medication mistakes occur at multiple points, including prescribing, dispensing, and administration.
Prescribing Errors

- A patient on warfarin who was prescribed a non-steroidal anti-inflammatory that increases bleeding risk
- A pediatric patient given an adult dose of medication
- Antibiotics prescribed to a patient despite documented allergies
- Immune suppressing drugs given to a patient suffering from an infection
Pharmacy Dispensing Errors
Pharmacists who fill prescriptions with the wrong medication or wrong strength, fail to counsel patients about side effects, or miss dangerous drug interactions share liability for resulting injuries. Look-alike and sound-alike drug names can lead to dispensing errors when pharmacists fail to carefully verify prescriptions.
Administration Errors
Hospital nurses who administer medications via the wrong route (IV instead of oral), at the wrong time, or to the wrong patient violate medication-administration protocols. Barcode scanning and double-check procedures prevent most administration errors, but shortcuts and distractions still cause preventable harm.
Birth Injuries and Obstetric Negligence
Labor and delivery complications, like shoulder dystocia, umbilical cord compression, placental abruption, and uterine rupture, require immediate recognition and intervention to prevent brain damage and death. Obstetricians, labor nurses, and neonatologists who fail to monitor fetal distress, delay emergency cesarean sections, or misuse delivery instruments cause permanent injuries to mothers and babies.
Failure to Monitor Fetal Distress
Electronic fetal monitoring tracks the baby’s heart rate and identifies patterns that suggest oxygen deprivation, including late decelerations, minimal variability, and prolonged bradycardia. Providers who misinterpret monitoring strips, fail to escalate care when tracings worsen, or don’t recognize non-reassuring patterns allow preventable brain injuries.
Delayed Cesarean Section
When vaginal delivery becomes dangerous, obstetricians must perform emergency cesarean sections quickly. The “decision-to-incision” time has a direct impact on outcomes. Delays caused by unavailable operating rooms, staffing shortages, or physician hesitation cause hypoxic-ischemic encephalopathy (HIE), cerebral palsy, and death.
Improper Use of Forceps and Vacuum Extractors
Forceps and vacuum extractors assist difficult deliveries but cause skull fractures, brain bleeds, and nerve damage when misused. Excessive traction, multiple pull attempts, or the use of instruments when contraindicated can create malpractice liability.
Maternal Injuries
Mothers suffer injuries during labor and delivery, too. This may include:
- Severe perineal tears
- Hemorrhage from uterine atony
- Infections from retained placental tissue
Providers who fail to repair lacerations properly, don’t recognize and treat post-partum hemorrhage promptly, or miss signs of infection cause long-term complications and sometimes death.
Failure to Obtain Informed Consent
Georgia law requires physicians to obtain informed consent before performing procedures, explaining the nature of the treatment, material risks, alternatives, and consequences of refusing treatment. Patients who undergo procedures without understanding risks, or who would have chosen differently if properly informed, may pursue lack-of-informed-consent claims even when the procedure was performed competently.
Georgia courts recognize that reasonable patients need access to material information to make informed healthcare decisions. “Material” means information that a reasonable person in the patient’s position would consider significant in deciding whether to proceed.
Providers who withhold risks, overstate benefits, or pressure patients into consenting deprive patients of autonomous medical decision-making.
Radiology and Laboratory Errors
Radiologists interpret imaging studies, including X-rays, CT scans, MRIs, and ultrasounds, while pathologists analyze tissue samples and laboratory results. Errors in reading films, delayed reporting of critical findings, or lost specimens cause diagnostic delays and treatment failures.
Missed Findings on Imaging
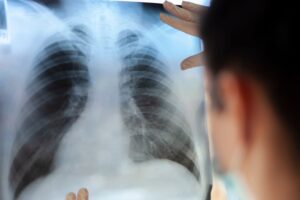
Peer review, double-reading high-risk studies, and structured reporting all reduce error rates.
Delayed Critical Results
A radiologist who identifies a life-threatening finding, but doesn’t immediately notify the ordering physician, commits negligence. Critical results policies require direct communication within minutes to hours, not simply filing a report that might sit unread in an electronic medical record for days.
Laboratory Mix-Ups
Specimens mislabeled, lost, or contaminated can produce false results, leading to incorrect treatments. A biopsy reported as benign when the tissue actually showed cancer, or blood-type errors that cause fatal transfusion reactions, all represent laboratory negligence.
Hospital-Acquired Infections
Infections contracted during hospital stays, such as surgical-site infections, catheter-associated urinary tract infections, central-line bloodstream infections, and ventilator-associated pneumonia, result from poor infection-control practices.
Hand hygiene, sterile technique during procedures, proper catheter care, and timely removal of invasive devices prevent the majority of hospital-acquired infections.
Providers who don’t follow CDC infection control guidelines, hospitals that tolerate noncompliance, or facilities with inadequate staffing that prevents proper cleaning and monitoring create conditions where preventable infections thrive. When these infections cause sepsis, prolonged hospitalization, additional surgeries, or death, the responsible providers and institutions can face liability.
Emergency Room Malpractice in Georgia
Georgia law treats emergency medical care differently from routine healthcare. O.C.G.A. § 51-1-29.5(c) requires plaintiffs to prove gross negligence. Gross negligence is characterized by willful and wanton misconduct or a conscious indifference to the consequences.
This higher standard recognizes the time pressure, incomplete information, and resource constraints emergency providers face. Discharging chest-pain patients without EKGs or troponin tests, sending head injury patients home without CT scans when clinical guidelines require imaging, or ignoring obvious signs of stroke or sepsis all may meet the gross-negligence threshold.
Emergency room malpractice cases require careful analysis of triage decisions, diagnostic testing, and discharge instructions to determine whether the provider’s conduct rose to the level of conscious indifference rather than mere misjudgment.
Georgia Medical Malpractice Expert Affidavit Requirement
Georgia imposes procedural requirements that distinguish medical malpractice claims from other personal injury cases, making early attorney involvement essential.
O.C.G.A. § 9-11-9.1 requires plaintiffs to file an expert affidavit with the complaint. This is a sworn statement from a qualified medical expert stating that the defendant’s care fell below the standard and caused injury. The expert must practice in the same specialty or hold relevant credentials.
Obtaining expert affidavits takes time. Experts must review complete medical records, research the standard of care, and prepare detailed opinions explaining how the defendant’s conduct deviated from accepted practice. This process requires weeks to months, making early case investigation critical to meet Georgia’s statute of limitations.
When to Consult a Kennesaw Medical Malpractice Lawyer
Medical malpractice cases require more thorough investigation, expert coordination, and legal analysis than other types of personal injury cases. Healthcare providers carry substantial malpractice insurance but defend claims aggressively with experienced defense lawyers and well-paid expert witnesses who testify that care met the standard.
Early consultation allows attorneys to preserve medical records before they’re altered or lost, identify appropriate expert witnesses in the defendant’s specialty, and analyze whether Georgia’s expert affidavit and statute of limitations requirements can be met.
Situations requiring immediate legal consultation include:
- Unexpected death or permanent disability following a medical treatment, surgery, or childbirth.
- Significant complications that were not disclosed as risks during informed-consent discussions.
- Diagnostic delays where earlier detection would have changed treatment options or prognosis.
- Emergency room discharges followed by a rapid deterioration requiring hospitalization or causing lasting harm.
- Birth injuries resulting in cerebral palsy, Erb’s palsy, or developmental delays.
Our medical malpractice lawyers offer free consultations to review medical records, explain Georgia’s malpractice laws, and connect you with qualified medical experts who evaluate whether the standard of care was breached. We handle medical malpractice cases on a contingency fee basis, meaning you pay nothing unless we recover compensation.
Frequently Asked Questions About Medical Malpractice in Georgia
O.C.G.A. § 9-3-71 gives you two years from the date of injury or discovery to file suit, with a five-year statute of repose barring claims filed more than five years after the negligent act, regardless of discovery. The two-year clock sometimes starts when you discover the injury rather than when it occurred, but the five-year absolute deadline always applies.
No. Georgia’s non-economic damages cap was struck down as unconstitutional in Nestlehutt v. Atlanta Oculoplastic Surgery, P.C. (2010). Juries decide pain and suffering awards without statutory limits, though the strength of your expert testimony and evidence about injury severity and life impact drives case value.
Not every bad outcome constitutes malpractice. Medicine involves inherent risks, and complications occur even when providers exercise reasonable care. Malpractice requires proof that the provider breached the standard of care and that the breach caused your injury.
Georgia law allows the deceased’s spouse, children, or parents to pursue wrongful death claims under O.C.G.A. § 51-4-2, recovering the value of the life lost, including income, benefits, and intangible loss of care and companionship. These claims are subject to the same two-year statute of limitations and expert affidavit requirements as other medical malpractice cases.
Yes. A provider’s admission strengthens your case but doesn’t eliminate Georgia’s expert-affidavit requirement under O.C.G.A. § 9-11-9.1 or the two-year statute of limitations.
Hold Georgia Healthcare Providers Accountable for Preventable Harm

Misdiagnosis, surgical errors, medication mistakes, birth injuries, and anesthesia complications cause preventable harm when healthcare providers breach the standard of care, but proving these claims demands thorough investigation, qualified medical experts, and experienced legal representation.
Williams Elleby Howard & Easter handles medical malpractice cases throughout Kennesaw and Cobb County. We review medical records, consult with experts in the defendant’s specialty, and build cases that meet Georgia’s expert-affidavit requirements. Our attorneys understand the law and how to present complex medical evidence to juries.
Call (404) 389-1035 or visit our contact page for a free consultation. We’ll review your medical records, explain Georgia’s malpractice laws, and fight to hold negligent providers accountable for the harm they caused.





